
科学研究
Original Research
JOURNAL:ACC Article Link
Gilbert Hin-Lung Tang, MD, MSC, MBA, FACC
Severe tricuspid regurgitation (TR), whether symptomatic or asymptomatic, is predictive of poor survival if left untreated. Medical therapy, consisting mostly of diuretics, is of limited efficacy. Clinical sequelae, including right heart dysfunction, peripheral edema, and liver congestion, confer a poor quality of life and poor prognosis. Surgical tricuspid repair and replacement have significant mortality and morbidity risks due to patient comorbidities and poor right heart function.
Transcatheter tricuspid valve repair is an emerging alternative to medical therapy and surgery to manage patients with symptomatic severe TR. Several technologies are currently in clinical trials, including edge-to-edge repair, annuloplasty repair, and de novo replacement (Figure 1). The MitraClip device (Abbott Structural Heart; Santa Clara, CA) has been used to repair the tricuspid valve in an off-label manner in over 1,000 cases worldwide with excellent safety and good efficacy, as evidenced by multicenter retrospective studies and the TriValve Registry. The TRILUMINATE (Evaluation of Treatment With Abbott Transcatheter Clip Repair System in Patients With Moderate or Greater Tricuspid Regurgitation) global feasibility study, consisting of sites from the European Union and United States, evaluated transcatheter tricuspid valve repair using the TriClip system (Abbott Structural Heart; Santa Clara, CA). The 1-year outcomes, presented at the 2019 PCR London Valves Annual Meeting, showed excellent safety and efficacy of the TriClip system in terms of TR reduction, low mortality, improvement in quality of life, and right atrial and ventricular modeling (Figures 2-3).1
Figure 1: Transcatheter Tricuspid Therapy Landscape
Figure 2
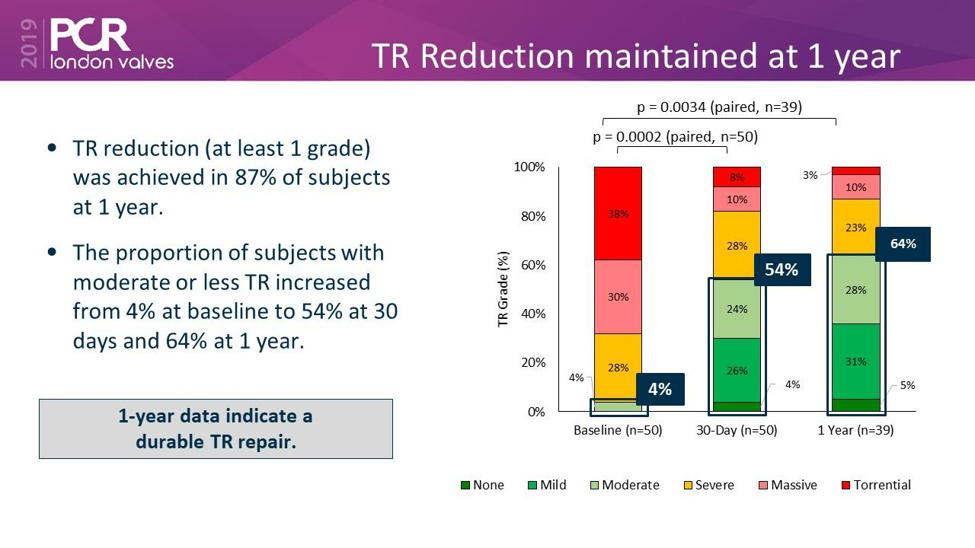
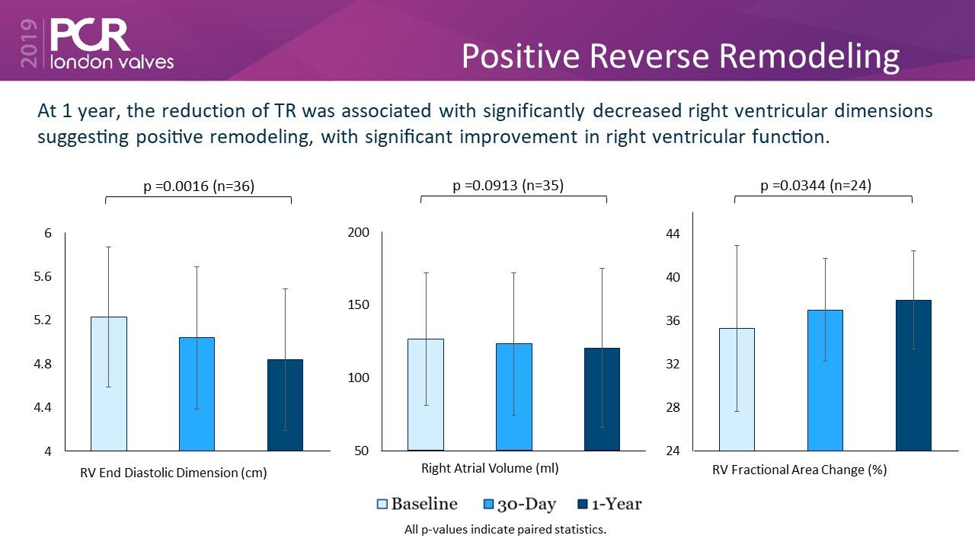
Figure 3
Imaging the tricuspid valve can be challenging. Transesophageal
echocardiography (TEE) is the primary modality used to optimize leaflet
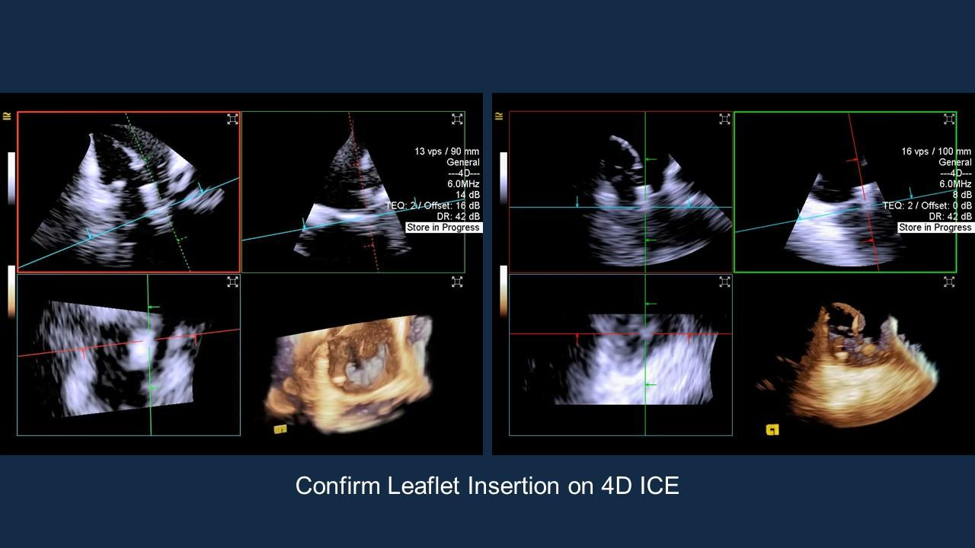
grasping and assessment of insertion (Figure 4). Intracardiac
echocardiography (ICE) can be a valuable complementary imaging tool to
confirm leaflet insertion (Figure 5).2 The TRILUMINATE
Pivotal Trial is currently ongoing, randomizing patients with
symptomatic severe TR to medical therapy or TriClip or utilizing TriClip
as a treatment arm if the TR can be reduced by only one grade in
severity.
Figure 4
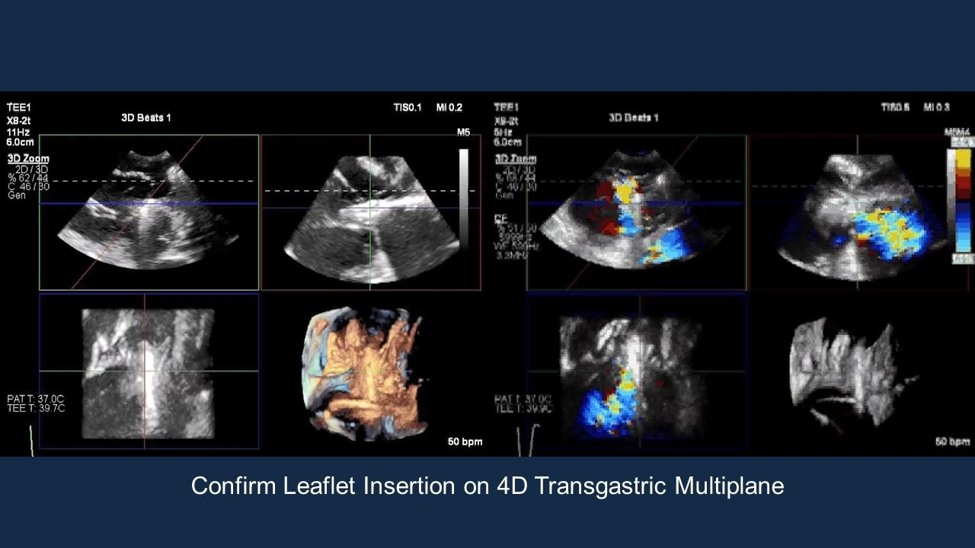
Figure 5
References